Page of Contents
What Is A Liver Fluke?
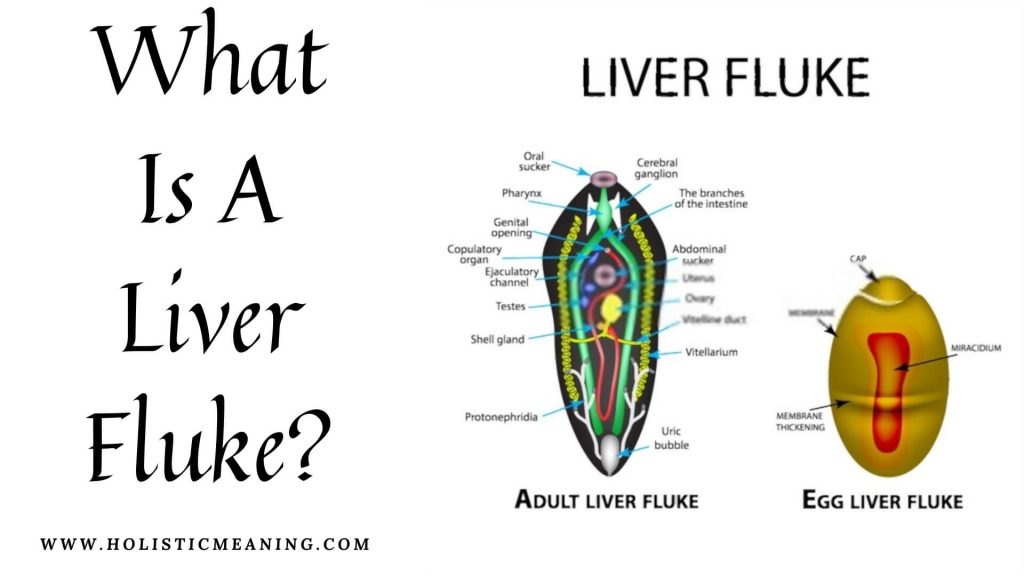
Topic: What Is A Liver Fluke?
The liver fluke is a parasite that can cause disease in humans and some animals. Read full article on What Is A Liver Fluke? below:
Liver fluke cannot be spread from person to person. Instead, people and animals become infected with the liver parasite from eating contaminated fish or drinking contaminated water.
The liver fluke, Fasciola hepatica, is a fluke parasite normally found in herbivores such as sheep, cows, and water buffalo, as well as some freshwater snails. It is apparently found on everywhere except Antarctica.
Herbivores shed eggs in their feces that hatch into larvae in fresh water in about 2 weeks. The larvae then infect freshwater snails where large numbers of more mature free-living larvae are produced and excreted into the water. These free-living larvae then attach themselves to aquatic plants where they encyst, called metacercariae, helping them survive if the plant dries out. Humans become infected after drinking water or eating aquatic plants contaminated with metacercariae, for example. watercress. There is no person-to-person transmission.
The mature flounder is typically around 10-15mm wide and 30mm long, although there is a less common species, Fasciola gigantica, which can grow up to 75mm long.
What Is A Liver Fluke In Humans?
The patient was a middle-aged man who was originally born in South America but had lived in the UK for several years. He made an appointment to see his GP when his wife noticed that his eyes had started to turn yellow. When he saw his GP, he clearly had jaundice, although he had no fever or abdominal pain, so infection was not suspected. The GP arranged for blood tests and an abdominal ultrasound to look for any obstruction in the biliary system that might explain the man’s symptoms. Blood tests confirmed elevated bilirubin and slightly abnormal live enzymes, but the total white blood cell count and CRP appeared normal. The ultrasound did not show gallstones (the most common cause of obstruction in the UK other than traffic jams!), But it did show a dilated common bile duct suggesting some form of obstruction.
The patient was mentioned a gastroenterologist for further investigation. After seeing the patient, the gastroenterologist wondered if he might have been in contact with a “funny infection” linked to his South American origin that could be the cause of jaundice and abnormal liver enzymes, and called the microbiologist to discuss the patient.
While talking on the phone, the microbiologist was reviewing the patient’s results and while the total white blood cells were in the normal range, the small part made up of eosinophils was actually removed.
“I wonder if this is often fascioliasis,” said the microbiologist, “you know of a Fasciola hepatica .”
“Actually?” the gastroenterologist replied, “You may have thwarted the diagnosis, but in the meantime, I’d better have an ERCP to make sure it’s not something more sinister like cancer or something.”
The gastroenterologist arranged for the shipment of three stool samples on consecutive days, as well as the blood test, and wrote a referral letter for ERCP (endoscopic retrograde cholangiopancreatography). Meanwhile, the lab got down to business looking at the poop!
What Is A Liver Fluke In Humans Stool?
The most common method of diagnosing fascioliasis is the detection of eggs in stool samples from infected patients, although these are only present in the chronic phase. It is best to run 3 samples on consecutive days so that the lab has the best chance of seeing the eggs. It is possible to get trapped by seeing eggs in the feces, as there is a condition known as “pseudo-fasciolosis” when eggs are seen in the feces after ingesting the liver of an infected animal. These eggs are not infectious (remember that only mature larvae are infectious), so it is important to follow a careful diet before collecting samples.
In the acute phase, before the eggs are present in the feces, serology can be performed to look for antibodies that indicate an immune response to the infection. This can also be done in the chronic phase, but it is important to remember that people in an endemic country can have positive serology if they have been infected and treated in the past.
How is fascioliasis treated?
The main treatment for fascioliasis is a drug called triclabendazole, which is given in a single dose of 10 mg / kg. It is not licensed for use in humans in the UK and must be obtained for each patient. I have been able to find over 40 different triclabendazole products listed on the internet for liver parasite treatment, but unfortunately they are all intended for animals! I was only able to find a product for human use called Egaten and made by Novartis.
It goes without saying that with so many products available for animals and the widespread use of triclabendazole to treat liver parasite in sheep and cattle around the world, there is now a growing problem with resistance to triclabendazole in liver parasite.
Another agent that may be effective in treating fascioliasis is another drug called Nitazoxanide. This drug is employed to treat other parasitic diseases in humans like cryptosporidiosis and giardiasis, so it’s known to be safe in humans.
The only problem is that there is no clear evidence that it works, it is only theoretical. Again, there are many products available for use in animals to treat parasitic diseases, so resistance can also be an issue with nitazoxanide. It is a difficult situation.
There are calls to reduce the amount of drugs used in livestock but on the other hand we do not want animals with infections, and when we buy meat or pate in supermarkets, nobody just wants to eat a plate of liver and find half a liver, stroke of luck left on your plate!.
So the patient sent stool samples to the lab and the biomedical scientist saw parasite eggs. These have been confirmed as Fasciola hepatica; serology also confirmed the diagnosis. The patient was treated with triclabendazole obtained from Novartis. To make sure nothing else happened, the patient underwent ERCP that did not confirm any other problems. After a few weeks, the patient’s jaundice completely disappeared.
The case showed up at the Grand Round Hospital at lunchtime and oddly enough there were a lot of partially eaten dishes left in the end … only microbiologists seem to be put off by that kind of story!
Leave a Reply